History of the Stethoscope

The first stethoscope
The stethoscope is a standardized examination tool in healthcare and a symbol of the medical profession. Whether conducting an annual checkup or a specialized treatment, the stethoscope plays a critical role in a clinician's ability to assess, diagnose, and monitor patients. However, the tried-and-true stethoscope of the past is being upgraded with new technologies to improve provider confidence and patient outcomes.
Prior to the stethoscope's invention, doctors placed their ears against patients' chests to evaluate their health in a process called immediate auscultation. This rudimentary method proved awkward for patient-clinician relationships, and in 1816, the French physician Rene Laennec conceived that a rolled piece of paper placed between the patient's chest and his ear could amplify heart sounds without requiring physical contact. This initial development led Laennec to develop the first stethoscope device which was almost named the cylinder due to its shape. Ultimately, Laennec settled on a stethoscope because stetho means chest and scope means viewing.

The first stethoscope was a hollow wooden monaural tube with a funnel at the end. It was placed in a clinician's ear in a process called mediate auscultation, because it provided a tool intermediate between the patient and clinician.
Later models
After Laennec's death, physicians began perfecting his design by adding earpieces so that bodily (auscultation) sounds could be heard in both ears. In 1851, Arthur Leared developed the first binaural stethoscope, and a year later in 1852, George Phillip Cammann created a flexible, rubber stethoscope for commercial use that resembles the one used today.

In the 1940s, Rappaport and Sprague modified the stethoscope further to create the two-sided chestpiece. With this design, one side was used for the respiratory system and the other was for the cardiovascular system. The model was heavy and short. It was also plagued by noise artifacts created when the two tubes rubbed together. It was later abandoned.
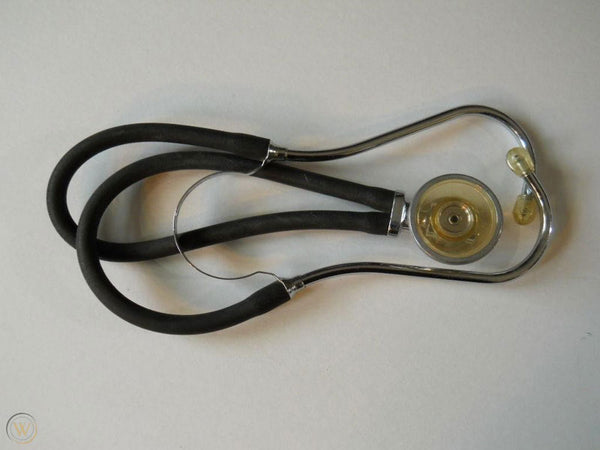
In the 1960s, Dr. David Littmann created a lighter stethoscope with a single tube, a tunable diaphragm, and better acoustics, which created the common diagnostic tool that we know today.

Types of stethoscopes
Stethoscopes are an undeniable symbol of healthcare professionals denoting trustworthiness and care. Here are some of the common types of stethoscopes:
- An acoustic (analog) stethoscope is the most common type of stethoscope which may be used for taking blood pressure, listening to the heart, lungs, veins, or bowels. Acoustic stethoscopes operate on the transmission of sound from the chest piece, via air-filled hollow tubes, to the listener's ears. The chestpiece usually consists of two sides that can be placed against the patient for sensing sound: a diaphragm (plastic disc) or bell (hollow cup). The bell transmits low-frequency sounds, while the diaphragm transmits higher frequency sounds. Unfortunately, the acoustic stethoscope's sound intensity is rather low, as there are no means of amplification or ambient noise reduction. The examples shown above are all acoustic stethoscopes.
- An electronic stethoscope amplifies and enhances sounds. These types of electronic stethoscopes filter analog sound and send it to the listener's ear via tubs.
- Digital stethoscope digitizes (converts) the analog signal and transmits it elsewhere for listening, storage, forwarding, and analysis.
- A fetal stethoscope is a trumpet that amplifies the sounds of a fetal heartbeat when placed against a mother's abdomen.
- A Doppler stethoscope is an electronic device that quantifies movement of body parts or fluids by transmitting ultrasound waves into the body and measuring the frequency shift of those sounds as they are reflected. This is called the Doppler effect. Doppler stethoscopes are particularly suited to deal with moving objects such as a beating heart.
The future of stethoscopes
The analog stethoscope has been a ubiquitous symbol of healthcare for over 200 years, but it is increasingly rarely used to its full potential. This is due to the substantial time required for proper training and the time required to maintain auscultation skills. As a result, this valuable diagnostic device has become underutilized. We concur with Dr. James Thomas, a cardiologist at Northwestern Medicine in Chicago, when he said, "the old stethoscope is kind of falling on hard times in terms of rigorous training. " The final nail in this coffin came on January 27, 2021, when the USMLE exam component that requires medical students to learn physical examination skills was permanently discontinued. As a result of this discontinuation, even a minimum level of physical exam proficiency can no longer be assured.
A lack of auscultation training and proficiency is troubling. Several recent studies have already shown that graduates in internal medicine and emergency medicine may miss as many as half of murmurs using a stethoscope. Furthermore, a comparative test of medical students, residents, fellows, and attending physicians has shown that auscultation skills peak in the middle of fellowship and decline thereafter, with competency scores ranging from 64% for medical students to 81% for cardiology fellows to 65% for private practice internal medicine attending physicians.
Added to this troubling situation is an incredible lack of evaluation time for providers. In 2018, approximately 33% of U.S. primary care physicians spent 17-24 minutes with their patients. It is simply not possible to conduct even a limited history assessment and physical examination in this short period while also discussing findings, the plan of care, and patients' questions. Yet patients still need to be evaluated and treated. In order to meet this need, healthcare providers now shift the diagnostic burden from the physical exam to ordering tests like echocardiograms and x-rays.
Unfortunately, ordering tests like these increases the complexity of care, cost, and inefficiency, and it hinders the tremendous value that listening to body sounds in a physical examination provides. However, by leveraging new technology, providers can analyze patient sounds and make treatment decisions quickly, even from a distance. These technologies allow providers to spend a short amount of time capturing those signals after which they will be digitally evaluated with artificial intelligence. The result is a workflow that provides a faster, more accurate, and more consistent evaluation.
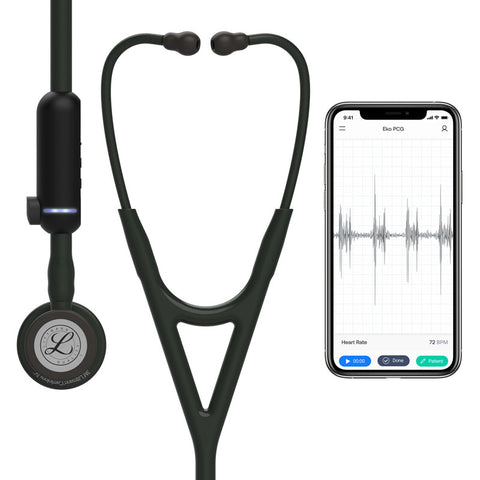
A new breed of advanced digital stethoscopes is the key to achieving this goal. Electronic stethoscopes augment analog stethoscopes with features like noise cancellation and amplification, and some electronic stethoscopes models will even store information. Digital stethoscopes that use artificial intelligence machine learning algorithms act as an information appliance that can recognize patterns and provide consistent and valuable insights into a patient's health. This process occurs so seamlessly that the insights are at the level of the most well-trained experts.
Digital stethoscopes are the future of stethoscopes and will change the landscape of the physical examination. Already, the first round of AI algorithms can detect patient abnormalities within seconds of sound and ECG capture. When AI detects arrhythmias, bradycardia, and tachycardia within seconds, these outputs alert providers and puts patients on the proper path of care. Further, AI analysis doesn't stand in the way of additional investigations such as echocardiography and x-ray imaging when more detailed information is needed. Healthcare providers and patients who use these new digital AI-supported stethoscopes will naturally prefer them; no analog acoustic stethoscope can compare.
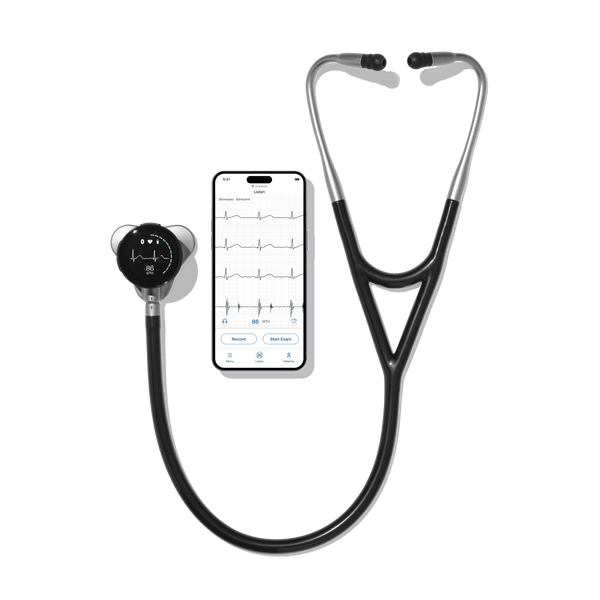
Current models of digital stethoscopes like the Eko CORE 500™ capture sound and electrical signals, and the first versions of AI-assistive algorithms work very well. In the future, the digital stethoscope will not be constrained by the historical model of what a stethoscope has been. It will constantly evolve to meet unmet clinical needs, and only be limited by technology and imagination.
